Atlanta Center for Gastroenterology, PC
& Atlanta Endoscopy Center, LTD
Offices of David Rausher, M.D., F.A.C.G., A.G.A.F., and Charles Parrish, M.D.

Understanding Heartburn / GERD (gastroesophageal reflux disease)
What Is GERD?
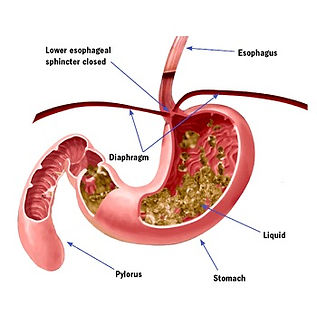
Gastroesophageal reflux disease (GERD) can be thought of as chronic symptoms of heartburn. The term refers to the frequent backing up (reflux) of stomach contents (food, acid, and/or bile) into the esophagus -- the tube that connects the throat to the stomach. GERD also refers to the array of medical complications, some serious, that can arise from this reflux.
Though it causes discomfort, occasional heartburn is not harmful. About 20% of adults in the U.S. experience GERD symptoms such as heartburn and acid regurgitation at least once a week. But if you have heartburn frequently and it is untreated, your stomach's acid may inflame the lining of your esophagus or swallowing tube, potentially narrowing it.
Stomach acid may also change the cells of the lining of your esophagus. This change, called Barrett's esophagus, increases the likelihood of cancer of the esophagus. Only a small percentage of people with GERD develop Barrett's esophagus.
Your stomach's contents can also move into your throat and be drawn past your vocal cords and into your lungs, where they can cause damage, along with hoarseness, a chronic dry cough, or asthma. Anyone can develop GERD at any age but you are more likely to develop it as you get older. Pregnant women are especially prone to GERD.
Heartburn and Reflux:
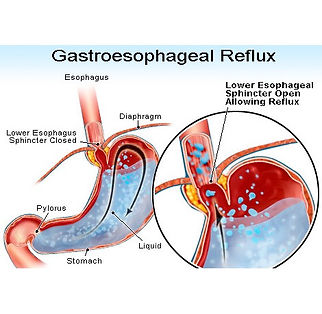
Heartburn is usually experienced as a burning sensation or pain behind the breastbone or a back up of bitter acid into the mouth. Ten percent of Americans experience it daily and 25 percent of pregnant women have heartburn. This discomfort is caused when the lower esophageal sphincter (LES) does not close properly and the stomach contents leak back into the esophagus.
What factors contribute to heartburn?
Most people experience heartburn after eating a large meal. Along with swallowed air, a large meal can increase pressure in the stomach, which overpowers the LES muscle. Other factors are: Nicotine (any tobacco products), Fried or fatty foods, Caffeine, Citrus fruits and juices, Peppermint and spearmint, Alcohol, Pregnancy, Lying flat, Hiatal hernia, and certain prescription medicines.
How is heartburn or reflux diagnosed?
Beyond the basic symptoms, there are several tests used to diagnose reflux:
Upper GI series- X-rays taken after you drink barium to monitor the esophagus and stomach.
Upper GI Endoscopy- After taking a mild sedative, a thin, lighted, flexible tube, called an endoscope, is inserted into the esophagus to visually inspect it and the stomach.
Esophageal Manometry- A test measuring pressure in the esophagus, especially the LES pressure.
pH Monitor- A test measuring how often stomach acid flows into the lower esophagus and the degree of acidity.
What is the treatment for heartburn and reflux?
An antacid or milk temporarily relieves heartburn for most people. However, the following measures are recommended for recurring reflux:
Antacids: These should be taken 30 - 60 minutes after eating and again at bedtime.
Drugs: Your doctor can prescribe medicines that reduce and eliminate the secretion of stomach acid and increase the strength of the LES muscle. The most potent of these are proton pump inhibitors.
Surgery: Surgery is rarely required to treat reflux. However, when antacids and drugs are ineffective, surgery (which can be performed laparoscopically) to strengthen the LES muscle must be considered.
Can I help keep reflux from recurring?
Eat smaller, more frequent meals.
Do not lie down immediately after eating, and avoid eating for several hours before going to bed.
Avoid excessive bending, lifting, abdominal exercises, girdles, and tight belts.
If you are overweight, lose weight.
Stop using all tobacco products.
Avoid fatty foods, alcohol, coffee, chocolate and peppermint.
Elevate the head of your bed eight to 10 inches so gravity can keep stomach juices out of your esophagus while you sleep. Extra pillows, by themselves, are usually sufficient.
Review all medications you are taking with your physician since certain prescription or over-the-counter medications can weaken the LES and aggravate reflux.
Can I expect complications from heartburn or reflux?
In some people, acid in the lower esophagus can lead to tissue damage, resulting in:
Chronic bleeding and anemia.
Scar formation and narrowing of the lower esophagus.
Barrett’s esophagus, which can occur when reflux irritates the lower esophagus over a long period of time and the lining of the stomach extends into the esophagus. This can be serious because it carries a slight risk of cancer developing.
Lung problems, which can develop if reflux causes stomach fluid to enter the breathing tubes
When should I call my physician?
Call your doctor if your heartburn is chronic and persistent.
GERD and Heart Disease
GERD can cause a crushing pain in your chest identical to the pain of a heart attack. Sometimes medical professionals diagnose GERD after evaluating a patient for repeated episodes of chest pain that are found to be unrelated to heart disease.
IMPORTANT! Never ignore pain in your chest. Seek immediate medical help. Call 911. A delay in getting help may be fatal. If your doctor says you have GERD, ask what to do if you have chest pain.
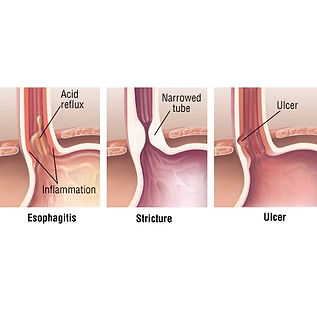
Esophagitis, Barrett's Esophagus, and Cancer of the Esophagus
Esophagitis, or inflammation of the esophagus, is a complication of GERD. If GERD is left untreated, esophagitis can cause bleeding, ulcers, and chronic scarring. This scarring can narrow the esophagus, eventually interfering with your ability to swallow.
One major complication which occurs in about 10% to 15% of people with chronic or longstanding GERD is Barrett's esophagus. Barrett's esophagus results when the normal cells of the esophagus are replaced with cells similar to those of the intestine. This increases the risk of esophageal cancer. Developing Barrett's esophagus does not mean you will get cancer, but your chances of getting cancer will be greatly increased. Your doctor will want to check you on a regular basis to detect any cancer in early stages. People with Barrett's may require periodic endoscopies with esophagus biopsies to check for pre-cancer cells (dysplasia).